- Главная
- Разное
- Дизайн
- Бизнес и предпринимательство
- Аналитика
- Образование
- Развлечения
- Красота и здоровье
- Финансы
- Государство
- Путешествия
- Спорт
- Недвижимость
- Армия
- Графика
- Культурология
- Еда и кулинария
- Лингвистика
- Английский язык
- Астрономия
- Алгебра
- Биология
- География
- Детские презентации
- Информатика
- История
- Литература
- Маркетинг
- Математика
- Медицина
- Менеджмент
- Музыка
- МХК
- Немецкий язык
- ОБЖ
- Обществознание
- Окружающий мир
- Педагогика
- Русский язык
- Технология
- Физика
- Философия
- Химия
- Шаблоны, картинки для презентаций
- Экология
- Экономика
- Юриспруденция
Colonic Polyps презентация
Содержание
- 1. Colonic Polyps
- 2. Colon Polyps The term polyp of
- 3. Non-neoplastic polyps Hyperplastic Mucosal
- 4. Hyperplastic polyps Located in the rectosigmoid
- 5. Hyperplastic polyposis syndrome (HPS) refers to
- 6. WHO criteria for HPS At
- 7. Mucosal polyps Mucosal polyps are small (usually
- 8. Inflammatory pseudo-polyps Inflammatory pseudopolyps are irregularly
- 9. Submucosal polyps Lymphoid aggregates, Lipomas,
- 10. Endoscopic Ultrasound Useful in defining the
- 11. Hamartomatous polyps Juvenile polyps Peutz-Jeghers polyps
- 12. Juvenile Polyps Juvenile polyps are hamartomatous
- 13. Familial Juvenile Polyposis FJP is associated
- 14. Peutz-Jeghers polyps The Peutz-Jeghers polyp is
- 15. Peutz-Jeghers polyps Patients with PJS are at
- 16. ADENOMATOUS POLYPS About two-thirds of
- 17. ADENOMATOUS POLYPS The time for development
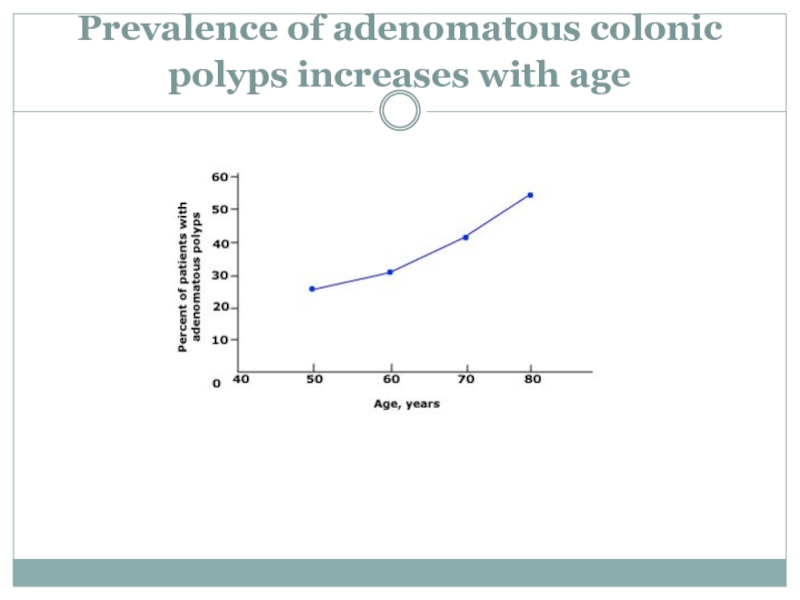
- 18. Prevalence of adenomatous colonic polyps increases with age
- 19. Synchronous lesion An adenoma that is
- 20. Metachronous lesion One that is
- 21. Pathologic classification The histologic features
- 22. Tubular adenomas Tubular adenomas account for more
- 23. Colonic adenoma
- 24. Villous adenomas Villous adenomas account for 5
- 25. Tubulovillous adenomas Tubulovillous adenomas account for
- 26. Polyp base Sessile - base is
- 27. Dysplasia All adenomas are dysplastic.
- 28. Invasive malignancy Invasive malignancy is defined by
- 29. Clinical presentation and natural history of
- 30. ADVANCED ADENOMA Villous histology,
- 31. Polyp size & advanced features The
- 32. Age & advanced features Older age
- 33. Advanced pathologic risk factors Adenomatous polyps
- 34. Detection and colonoscopic removal of polyps
- 35. Detection and colonoscopic removal of polyps
- 36. Prevention Guidelines proposed by American College
- 37. Surveillance Patients with small rectal hyperplastic
- 38. Surveillance Patients with only 1 or 2 small (
- 39. Surveillance Patients with multiple (3-10) adenomas,
- 40. Surveillance Patients who have more
- 41. Surveillance Patients with sessile adenomas
- 42. Hereditary nonpolyposis colorectal cancer Colonoscopy every
- 43. Familial Adenomatous Polyposis Colonoscopy every 12
Слайд 2Colon Polyps
The term polyp of the colon refers to a protuberance
into the lumen from the normally flat colonic mucosa.
Polyps are usually asymptomatic but may ulcerate and bleed, cause tenesmus if in the rectum, and, when very large, produce intestinal obstruction.
Polyps are usually asymptomatic but may ulcerate and bleed, cause tenesmus if in the rectum, and, when very large, produce intestinal obstruction.
Слайд 3Non-neoplastic polyps
Hyperplastic
Mucosal
Inflammatory
Submucosal
Adenomatous
Serrated –mixed hyperplastic and adenomatous
Hamartomous
Слайд 4Hyperplastic polyps
Located in the rectosigmoid
< 5 mm in size
Rarely
develop into colorectal cancers
Слайд 5Hyperplastic polyposis syndrome
(HPS) refers to a condition characterized by multiple, large
and/or proximal hyperplastic polyps and/or serrated adenomas - mixed hyperplastic / adenomatous polyps.
Слайд 6
WHO criteria for HPS
At least five hyperplastic polyps proximal to the
sigmoid colon, of which two are greater than 1 cm in diameter, or
Any number of hyperplastic polyps occurring proximal to the sigmoid colon in an individual who has a first degree relative with hyperplastic polyposis, or
Greater than 30 hyperplastic polyps distributed throughout the colon.
Any number of hyperplastic polyps occurring proximal to the sigmoid colon in an individual who has a first degree relative with hyperplastic polyposis, or
Greater than 30 hyperplastic polyps distributed throughout the colon.
Слайд 7Mucosal polyps
Mucosal polyps are small (usually
that endoscopically resemble the adjacent flat mucosa and histologically are normal mucosa. They have no clinical significance
Слайд 8Inflammatory pseudo-polyps
Inflammatory pseudopolyps are irregularly shaped islands of residual intact colonic
mucosa that are the result of the mucosal ulceration and regeneration that occurs in inflammatory bowel disease (IBD).
Typically multiple, often filiform and scattered throughout the colitic region of the colon. They may also be more isolated and semipedunculated in areas of more active recent inflammation, and have mucus adherent to their apices
Typically multiple, often filiform and scattered throughout the colitic region of the colon. They may also be more isolated and semipedunculated in areas of more active recent inflammation, and have mucus adherent to their apices
Слайд 9Submucosal polyps
Lymphoid aggregates,
Lipomas,
Leiomyomas,
Pneumatosis cystoid intestinalis,
Hemangiomas,
Fibromas,
Carcinoids,
Metastatic lesions
Слайд 10Endoscopic Ultrasound
Useful in defining the site of origin and for biopsy
of sub-mucosal lesions if the diagnosis is in doubt
Слайд 12Juvenile Polyps
Juvenile polyps are hamartomatous lesions that consist of a lamina
propria and dilated cystic glands rather than increased numbers of epithelial cells
Слайд 13Familial Juvenile Polyposis
FJP is associated with an increased risk for the
development of colorectal cancer, and in some families, gastric cancer, especially where there are both upper and lower gastrointestinal polyps.
Слайд 14Peutz-Jeghers polyps
The Peutz-Jeghers polyp is a hamartomatous lesion of glandular epithelium
supported by smooth muscle cells that is contiguous with the muscularis mucosa
Слайд 15Peutz-Jeghers polyps
Patients with PJS are at increased risk of both gastrointestinal
(gastric, small bowel, colon, pancreas) and nongastrointestinal cancers with a cumulative cancer risk of about 50 percent by age 60.
Слайд 16ADENOMATOUS POLYPS
About two-thirds of all colonic polyps are adenomas.
Adenomas
are by definition dysplastic and thus have malignant potential.
Nearly all colorectal cancers arise from adenomas, but only a small minority of adenomas progress to cancer (1 in 20 or less).
Nearly all colorectal cancers arise from adenomas, but only a small minority of adenomas progress to cancer (1 in 20 or less).
Слайд 17ADENOMATOUS POLYPS
The time for development of adenomas to cancer is about
seven years.
Approximately 30 to 40 percent of the United States population over the age of 50 have one or more adenomas
The cumulative colorectal cancer risk is about 5 percent.
Approximately 30 to 40 percent of the United States population over the age of 50 have one or more adenomas
The cumulative colorectal cancer risk is about 5 percent.
Слайд 19Synchronous lesion
An adenoma that is diagnosed at the same time as
an index colorectal neoplasm is called a synchronous lesion.
Thirty to 50 percent of colons with one adenoma will contain at least one other synchronous adenoma.
Thirty to 50 percent of colons with one adenoma will contain at least one other synchronous adenoma.
Слайд 20Metachronous lesion
One that is diagnosed at least six months later is
considered metachronous lesion
Слайд 21Pathologic classification
The histologic features and size of colonic adenomas are
the major determinants of their malignant potential.
The glandular architecture of adenomas is characterized as tubular, villous, or a mixture of the two.
The glandular architecture of adenomas is characterized as tubular, villous, or a mixture of the two.
Слайд 22Tubular adenomas
Tubular adenomas account for more than 80 percent of colonic
adenomas.
They are characterized by a network of branching adenomatous epithelium.
To be classified as tubular, the adenoma should have a tubular component of at least 75 percent
They are characterized by a network of branching adenomatous epithelium.
To be classified as tubular, the adenoma should have a tubular component of at least 75 percent
Слайд 24Villous adenomas
Villous adenomas account for 5 to 15 percent of adenomas.
They are characterized by glands that are long and extend straight down from the surface to the center of the polyp.
To be classified as villous, the adenoma should have a villous component of at least 75 percent.
Слайд 25Tubulovillous adenomas
Tubulovillous adenomas account for 5 to 15 percent of adenomas.
Have 26 to 75 percent villous component.
Слайд 26Polyp base
Sessile - base is attached to the colon wall,
Pedunculated
if a mucosal stalk is interposed between the polyp and the wall.
Adenomas are most commonly found within raised lesions, up to 27 to 36 percent are flat (having a height less than one-half the diameter of the lesion) and up to 1 percent are depressed
Adenomas are most commonly found within raised lesions, up to 27 to 36 percent are flat (having a height less than one-half the diameter of the lesion) and up to 1 percent are depressed
Слайд 27Dysplasia
All adenomas are dysplastic.
A new system that recognizes two grades
of dysplasia - HIGH and LOW.
Similarly, the older terms "carcinoma in situ" or "intramucosal adenocarcinoma" should both be described as high-grade dysplasia
Similarly, the older terms "carcinoma in situ" or "intramucosal adenocarcinoma" should both be described as high-grade dysplasia
Слайд 28Invasive malignancy
Invasive malignancy is defined by a breach of the muscularis
mucosa by neoplastic cells.
Because there are no lymphatic vessels in the lamina propria, they are not associated with metastasis, and can be managed along conventional guidelines in adenoma follow
Because there are no lymphatic vessels in the lamina propria, they are not associated with metastasis, and can be managed along conventional guidelines in adenoma follow
Слайд 29Clinical presentation and
natural history of Adenomas
Adenomas are generally asymptomatic and
are most often detected by colon cancer screening tests.
Small adenomas do not typically bleed
Adenomas are found in 17 to 43 percent of patients with a positive FOBT but they are also detected in 32 to 41 percent of asymptomatic men with a negative FOBT .
Advanced adenomas are more likely to bleed and cause a positive fecal occult blood test.
Small adenomas do not typically bleed
Adenomas are found in 17 to 43 percent of patients with a positive FOBT but they are also detected in 32 to 41 percent of asymptomatic men with a negative FOBT .
Advanced adenomas are more likely to bleed and cause a positive fecal occult blood test.
Слайд 31Polyp size & advanced features
The proportion of adenomas showing advanced histologic
features (high-grade dysplasia or >25 percent villous histology) increases from
1 % in small adenomas (<5 mm) to
7 to 12 % for medium-sized adenomas (5 to 10 mm)
20 % for large adenomas (>1 cm)
1 % in small adenomas (<5 mm) to
7 to 12 % for medium-sized adenomas (5 to 10 mm)
20 % for large adenomas (>1 cm)
Слайд 32Age & advanced features
Older age is also associated with high-grade dysplasia
within an adenoma, independent of size and histology
Слайд 33Advanced pathologic risk factors
Adenomatous polyps >1 cm in diameter
Adenomatous polyps
with high-grade dysplasia
Adenomatous polyps with >25 percent villous histology
Adenomatous polyps with invasive cancer
More than 2 adenomatous polyps
Adenomatous polyps with >25 percent villous histology
Adenomatous polyps with invasive cancer
More than 2 adenomatous polyps
Слайд 34Detection and colonoscopic removal of polyps
Colonoscopy is considered the optimal examination
for the detection of adenomatous polyps, particularly in view of the ability to provide therapeutic polypectomy in conjunction with diagnosis
Слайд 35Detection and colonoscopic removal of polyps
The colonoscopic miss rate determined by
two same day endoscopic examinations in 183 patients was
27 percent for adenomas <5 mm,
13 percent for those 6 to 9 mm, and
6 percent for adenomas >1 cm
27 percent for adenomas <5 mm,
13 percent for those 6 to 9 mm, and
6 percent for adenomas >1 cm
Слайд 36Prevention
Guidelines proposed by American College of Gastroenterology (ACG):
A diet that is
low in fat and high in fruits, vegetables, and fiber. There may be advantages with cruciferous vegetables and unprocessed forms of cereal fiber.
Maintenance of normal body weight through regular exercise and caloric restriction.
Avoidance of smoking and excessive alcohol use, especially beer.
Dietary supplementation with 3 g of Calcium Carbonate.
Maintenance of normal body weight through regular exercise and caloric restriction.
Avoidance of smoking and excessive alcohol use, especially beer.
Dietary supplementation with 3 g of Calcium Carbonate.
Слайд 37Surveillance
Patients with small rectal hyperplastic polyps should be considered to have
normal colonoscopies, and therefore the interval before the subsequent colonoscopy should be 10 years;
Слайд 38Surveillance
Patients with
only 1 or 2
small (
only low-grade dysplasia
should have their follow-up colonoscopy in
5-10 years.
Слайд 39Surveillance
Patients with
multiple (3-10) adenomas,
adenoma > 1 cm,
adenoma with
villous features,
high-grade dysplasia
should have their follow-up colonoscopy in 3 years providing that piecemeal removal has not been performed and the adenoma(s) are removed completely;
high-grade dysplasia
should have their follow-up colonoscopy in 3 years providing that piecemeal removal has not been performed and the adenoma(s) are removed completely;
Слайд 40Surveillance
Patients who have
more than 10 adenomas at 1 examination
should
be examined at a shorter (<3 y)
interval, established by clinical judgment,
and the clinician should consider the
possibility of an underlying familial
syndrome
interval, established by clinical judgment,
and the clinician should consider the
possibility of an underlying familial
syndrome
Слайд 41Surveillance
Patients with
sessile adenomas
that are removed piecemeal
should be considered
for follow-up
evaluation at short intervals (2-6 mo) to
verify complete removal;
evaluation at short intervals (2-6 mo) to
verify complete removal;
Слайд 42Hereditary nonpolyposis colorectal cancer
Colonoscopy every one to two years beginning at
age 20 to 25, or 10 years earlier than the youngest age of colon cancer diagnosis in the family (whichever comes first).
Слайд 43Familial Adenomatous Polyposis
Colonoscopy every 12 months starting at around age 10
to 12 and continuing until age 35 to 40 if negative.